Approximately 20 million people live with rheumatoid arthritis worldwide, and about a million new patients are diagnosed each year.1 As the population ages the prevalence of rheumatoid arthritis is expected to rise, and women are disproportionately affected.2
Early detection, treatment and proper disease management are crucial to slowing joint damage and avoiding complications like loss of movement and joint replacement, as well as other related outcomes like lost employment and premature heart disease.3 While it’s impossible to know how a specific patient's disease will progress, data collected by digital allows providers to be proactive and track trends over time to more accurately project disease progression.
Leading biopharma companies recognize the opportunity for digital to augment medications and manage disease progression for many conditions, including rheumatoid arthritis. In a recent survey conducted by BrightInsight and HealthXL, 61% of respondents said that disease management is the most promising use case for Software as a Medical Device (SaMD), and rheumatoid arthritis was named as a top 10 indication for SaMD. It’s no surprise as several biopharma companies have invested in R&D for rheumatoid arthritis and have drug candidates in the late clinical-stage of development.
[Rheumatoid arthritis] is still unclear to healthcare providers. They have 10 to 12 DMARDS and 6 different mechanisms of action, so which patient will respond better to which therapy? Yes—an algorithm in a disease management solution would be incredibly helpful."
- VP, Therapy Lead, Top 20 Biopharma company
Digital disease management solutions can directly drive therapy value in a multitude of ways: impacting physician prescribing patterns, improving patient access, increasing adherence or persistence and optimizing dose delivery, among others.
Digital enables more engaging patient experiences by increasing therapy compliance, improving disease and medical tracking and as importantly, building connections among patients and with healthcare providers. The data collected with digital can be used to deliver more personalized therapies, increase reimbursement and potentially increase revenues through extended patent life."
– Brad Gescheider, Global Head, Digital Innovation and Patient Services, Immunology at Sanofi
Digital solutions can help solve some of the challenges that have long impacted care for patients with rheumatoid arthritis. Here are some of the key obstacles:
Things don't change in a day for my patients, so [with a digital solution] I could plot what’s happening between visits, to see what’s happening over time."
- Immunologist
These challenges frustrate providers and patients alike, and bleed value from the healthcare system. Well-designed digital solutions can address these shortcomings by connecting healthcare stakeholders and giving them tools to excel. Successful digital solutions restore value in three important ways:
We should be growing faster, acquiring more patients. Marketing budget is not enough to solve upstream challenges. Relying on TV ads is a brute force approach, but what is required is a surgical approach: How do we get patients paired with the right doctor, healthcare system and drug? It takes time and resources, but the brand lifecycle is finite. How do you get more patients on your brand? Digital."
– Data Science & Artificial Intelligence lead at a top 10 biopharma company
In order to solve these disease management challenges and take advantage of the wide range of opportunities, it’s important to take a strategic approach. Here are some of the benefits our Disease Management Solution can deliver:
Applications that are configurable to meet your unique needs are core to both accelerating speed to market and expanding your product portfolio over time. Ensure that your platform of choice supports:
It’s also important to build on a platform that’s compliant with even the most highly regulated digital health SaMD classifications. This allows you to maintain compliance across geographies and over time, even as the product scales and evolves.
HEALTHCARE PROVIDER INTERFACES
Our Healthcare Provider Interfaces enable clinicians to facilitate improved communication with patients, and to see trend data directly within the EHR workflow to track how patients are responding to therapy.
A patient app with tools that support patients throughout their disease management journey is a key differentiator. A great patient app solution helps patients recognize the impact of their actions through features like symptom tracking, patient-care team communication, automated medication and refill reminders and integration with connected devices.
The best patient tools include personalized drug dosing algorithms to drive adherence and persistence, plus personalized education tools designed to empower patients.
CLINICAL RHEUMATOID ARTHRITIS ASSESSMENTS
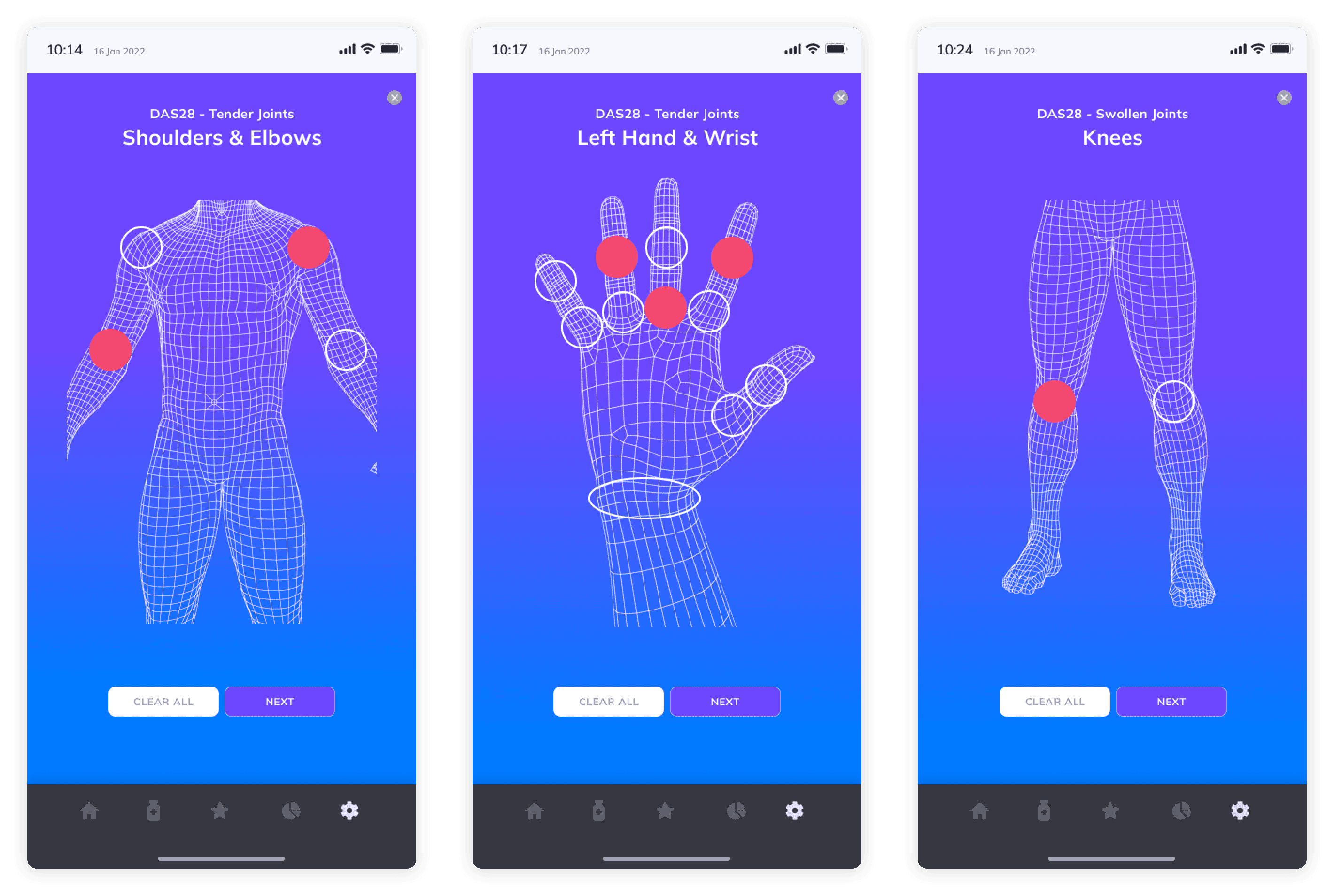
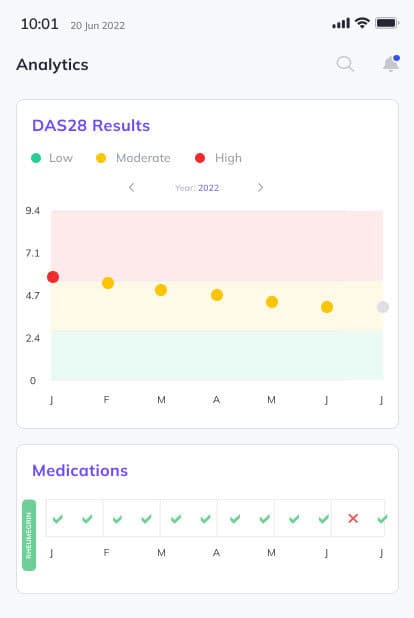
The Patient App connects patients to tools like clinical assessments, such as the DAS28 to assess RA disease activity level severity.
MEDICATION REMINDERS
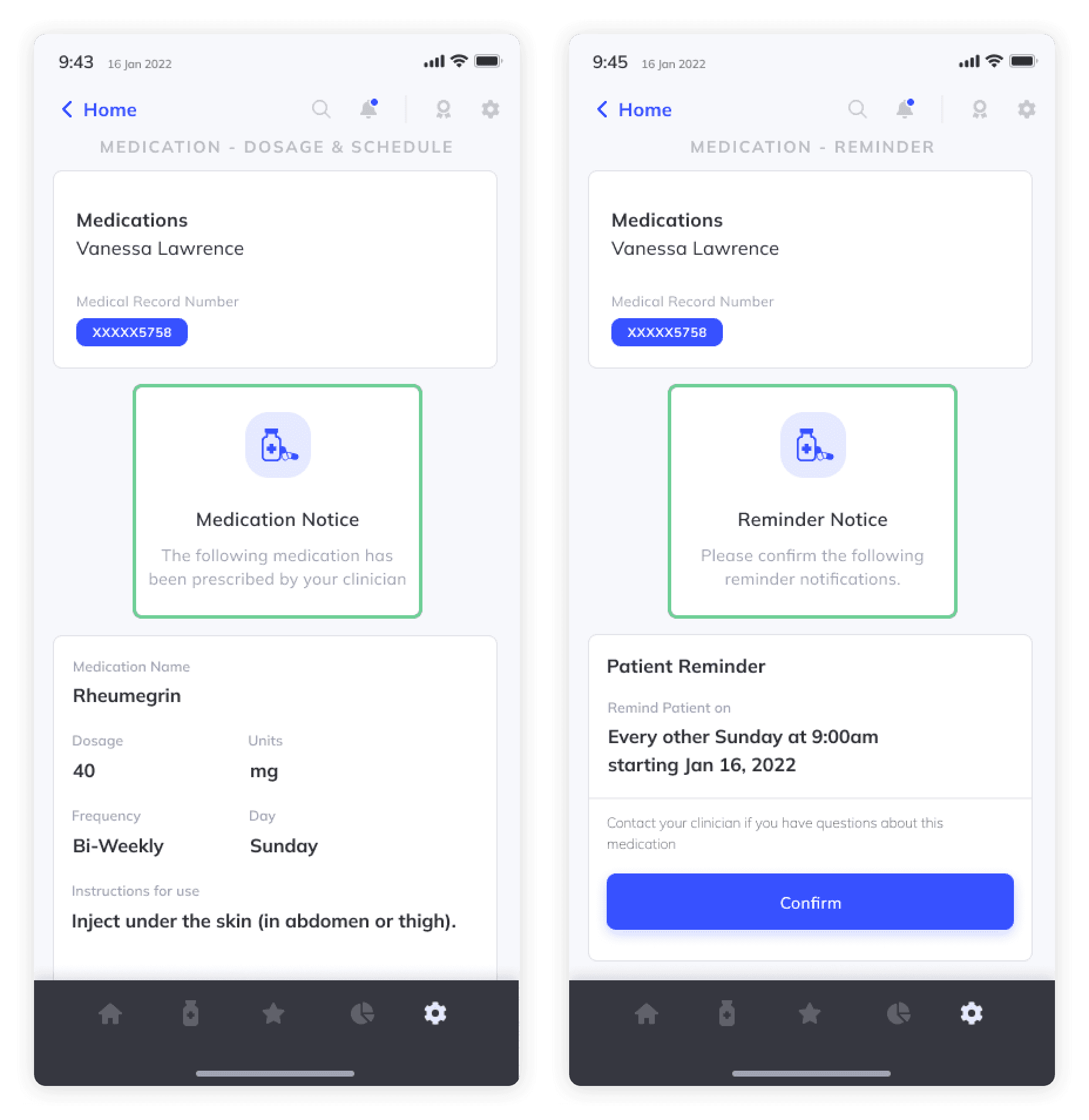
The BrightInsight Disease Management Solution imports a patient's RA therapy prescription directly from the EHR into their Patient App and medication reminders can be configured to support treatment persistence and adherence.
The most powerful digital health solutions allow for the secure, compliant capture and use of patient- and population-level data. On an individual level, analytics dashboards with usage and usability metrics, combined with algorithm hosting, aid clinical decision-making, increasing patient adoption and engagement. On a broader level, data powers reimbursement management tools, demonstrating therapy value to payers and increasing therapy access.
It’s a game changer if it creates less time for me to spend in the office. The common thread is patient engagement and participation in their treatment and journey. It's important to put the patient first and make them feel like they are useful in the process. That powerful sense of engagement says it all for them to participate. To objectively show them numbers, results—follow the disease progression through the journey. As a clinician, I welcome it—it's not easy to help them understand why we’re doing what we’re doing."
– Rheumatologist
ANALYTICS DASHBOARDS
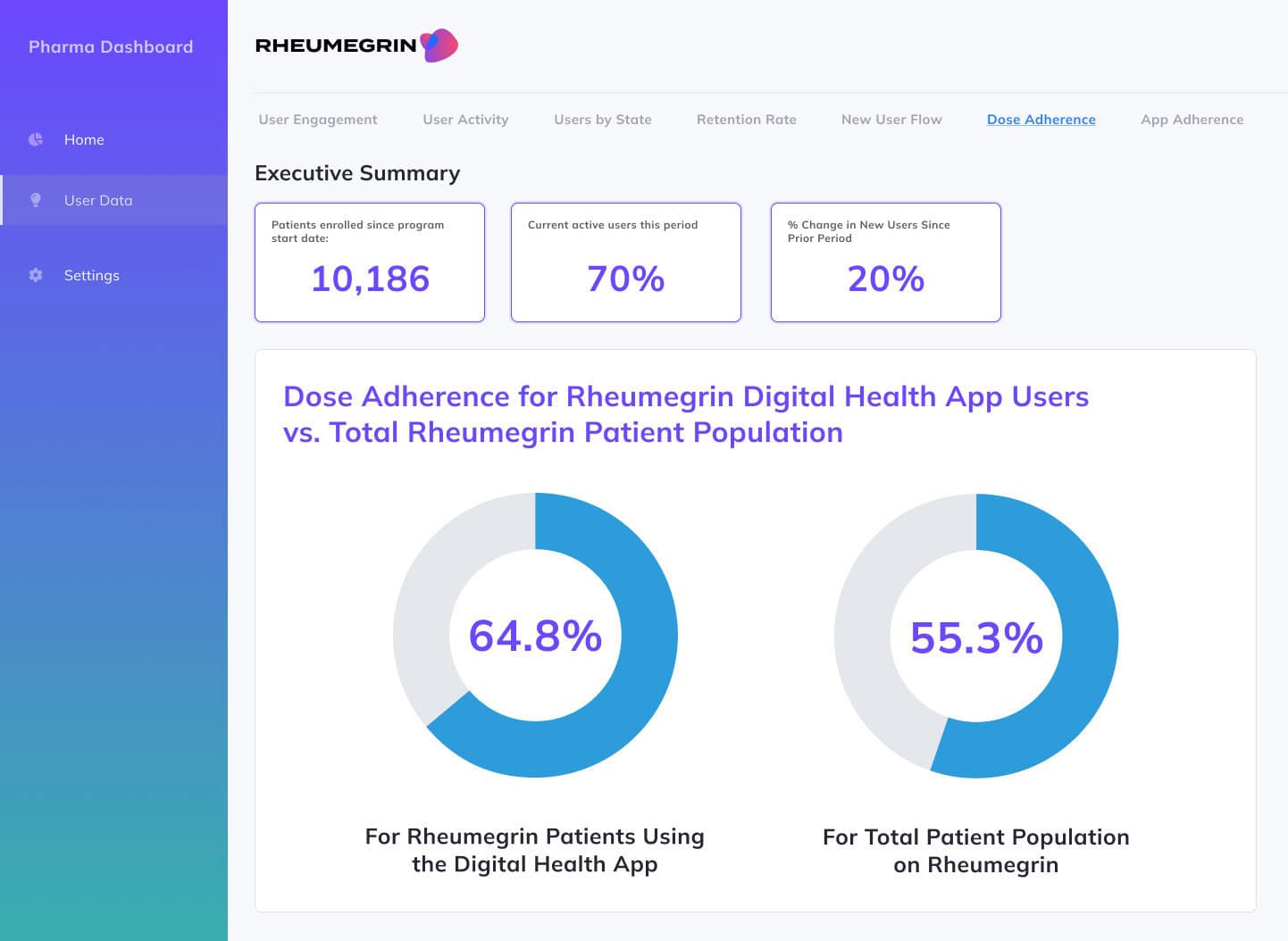
Commercial and brand leaders leverage our Analytics Dashboards to harness unique data to drive product strategy and marketing tactics.
Go with the proven partner that top biopharma companies trust. When you team up with BrightInsight, you can accelerate time to market while future-proofing your disease management solutions for regulatory, security and privacy compliance.
By building their disease management solutions on top of the BrightInsight® Platform, top biopharma companies can address patient and provider pain points and unlock a better path to adherence and persistence across a wide range of therapy areas and treatments.
The BrightInsight Disease Management Solution (DMS) is not a cleared or approved medical device. The use cases presented within this article are hypothetical use cases and do not make reference to a specific product, product claims, or product branding. The Rheumagrin interface that is illustrated is for example purposes only and does not represent a real product or product branding.